
19, 20 It has further been proposed that home self-treatment become an accepted part of the otolaryngologist's management of recurrent BPPV. Some authors have suggested that home self-treatment may be an alternative to clinician-guided repositioning. Both singular neurectomy and posterior semicircular canal occlusion are highly effective surgical procedures, though the latter is easier and carries less risk. 16 Beyond repositioning maneuvers, there is no effective nonsurgical treatment for BPPV. At our institution, we use a variation of the Epley maneuver that we call the particle repositioning maneuver (PRM). After the description of new repositioning maneuvers by Semont et al 2 in 1988 and Epley 3 in 1992, effective treatments for most patients became available ( Figure 1). However, these exercises required the regular induction of vertigo. In the 1980s, Brandt and Daroff 14 and Brandt et al 15 described a series of exercises that led to a more rapid resolution of symptoms. 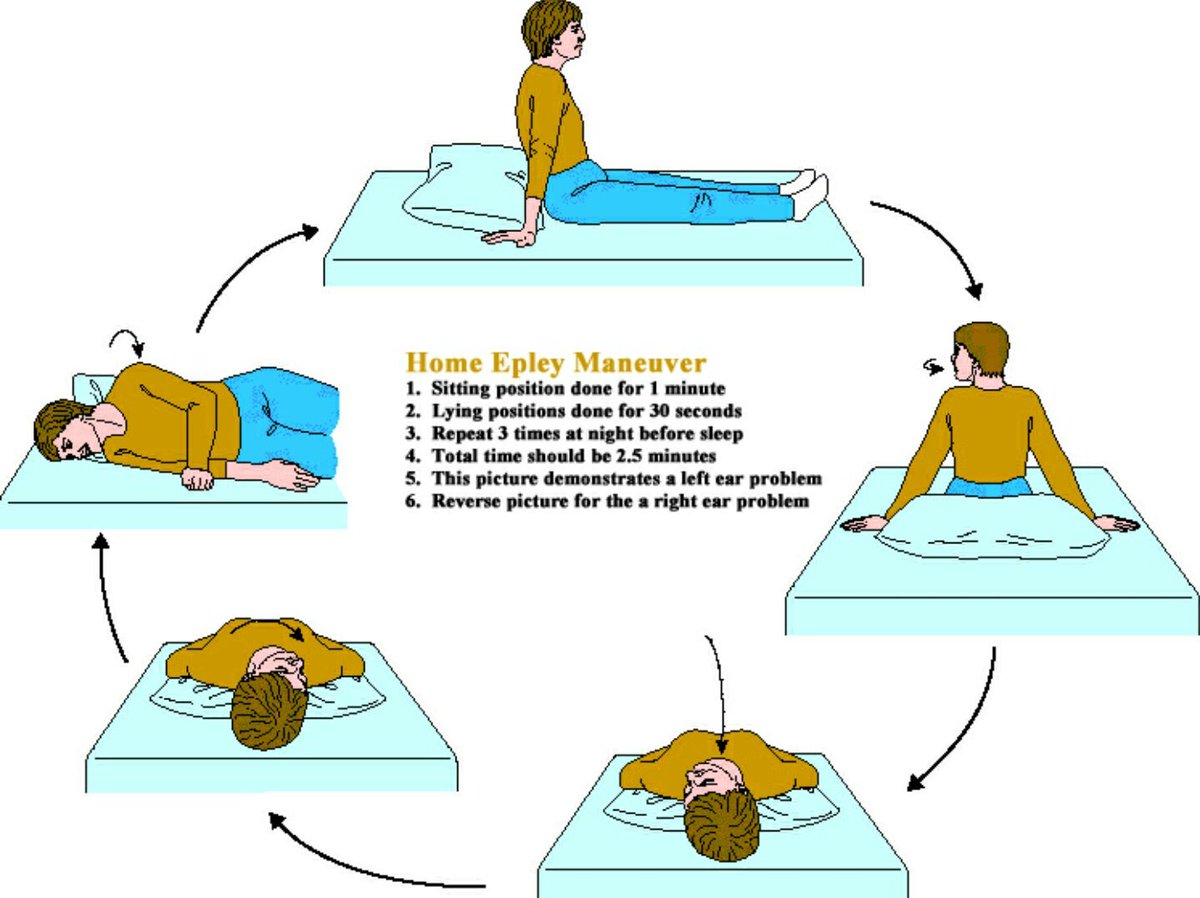
However, recurrence has been reported in as many as 30% to 50% of patients who undergo treatment by repositioning. 11 - 13 Reported recurrence rates vary widely and are dependent on the duration of follow-up. The incidence of BPPV increases with age and has been estimated at greater than 10% to 20% beyond the sixth decade of life. 5 While BPPV itself tends to resolve over weeks to months, the associated morbidity is high due to depression, anxiety, injury from falls, and occupational hazard. Superior canal BPPV, although rare, has downbeating vertical nystagmus. By contrast, horizontal BPPV has only horizontal nystagmus, which is either geotropic (fast component toward the ground) or apogeotropic (fast component away from the ground), depending on the variant. The nystagmus that occurs during posterior canal BPPV has characteristic upbeating and torsional components causing the superior pole of the eye to rotate toward the affected side in the head-hanging position. Short-lived nystagmus with associated vertigo results from gravity-induced movement of these particles. The current understanding of BPPV is that it occurs when otoconia become dislodged from the macula of the utricle and migrate down into the most gravity-dependent long arm of the posterior semicircular canal. 3 Following either, the condition is highly recurrent. The 2 fundamental maneuver variations are based on the techniques of Semont et al 2 and Epley. 1 Though it typically resolves over several months without any treatment, a clinician-guided maneuver can expedite the process.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
